Our Services
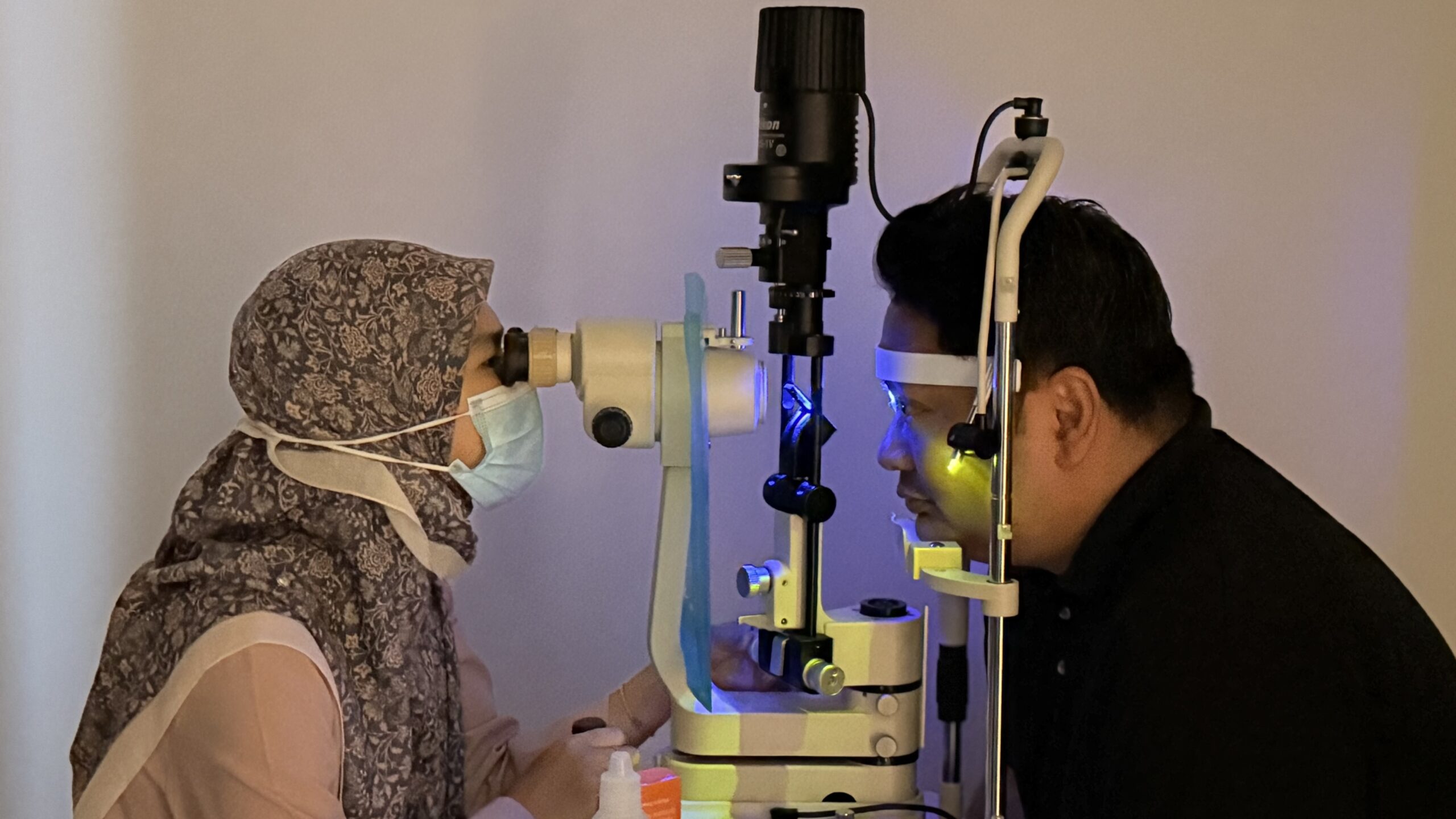
Glaucoma Screening
Glaucoma is an eye condition, usually due to a buildup of pressure inside the eye (intraocular pressure). The increased pressure can damage the optic nerve which connects the eyes to the brain. Unfortunately, the damage caused by glaucoma is irreversible. If the damage worsens, glaucoma can cause vision loss or even total blindness within a few years. Therefore, early diagnosis and treatment are crucial in preventing further damage and preserving your vision as much as possible.
Individuals with a family history of glaucoma, diabetes, or high blood pressure should have a comprehensive eye exam with an ophthalmologist or an optometrist more frequently i.e. every 1 year to 2 years after age 35. The American Academy of Ophthalmology recommends that adults with no sign or risk factors for eye disease including glaucoma to get a baseline eye disease screening at age 40. The risk for glaucoma increases with age. As such, for those age 65 years and older should get a comprehensive eye tests including glaucoma screening every 6 months to 1 year.
Glaucoma Screening involves a series of tests which include:
- Optic nerve assessment – to examine the health and appearance of the optic nerve at the back of the eye.
- Ocular pressure test (Tonometry) – uses a tonometer to measure the pressure inside the eye (intraocular pressure measurement).
- Gonioscopy – to check the fluid-filled space between the iris and cornea, and to determine whether the drainage angle where the fluid flow from the eye is clear or blocked. This will tell what type of glaucoma you have.
- Optical coherence tomography (OCT) – to look for changes in your optic nerve that may mean glaucoma.
- Visual Field Test – helps detect vision loss, a key indicator of glaucoma damage.
- Ophthalmoscopy – to examine the back of the eye (fundus) to assess the optic nerve and other structures.
Glaucoma requires lifelong management and regular checkups by the Ophthalmologist (eye doctor) to monitor the condition and adjust the treatment as needed. Glaucoma treatment primarily aims to lower intraocular pressure to prevent further optic nerve damage and vision loss. Among the common treatment methods are eye drops, laser treatments, or surgery.
Keratoconus Screening
Keratoconus is an eye condition in which the cornea (i.e. the clear, dome-shaped front surface of the eye) starts to thin and bulge outward into a cone shape. This affects the way light enters the eye and leads to sensitivity to glares, distorted and blurred vision. If left untreated, the condition will worsen over time.
This eye disease affects approximately 1/2000 people of all races and both sexes equally. Till now, eye doctors and researchers do not know exactly what causes keratoconus. In some cases, it may be linked to:
- Genetic: Those with family history of having this condition.
- Age: More common in adolescents and young adults than in older adults.
- Excessive eye rubbing over time can cause the cornea to break down.
- Certain connective tissue disorders e.g. Marfan syndrome, Ehlers-Danlos syndrome; and inflammation from allergies, asthma and atopic eye disease.
- Down Syndrome: 5%-30% of those born with Down Syndrome are likely to have thinner and less rounded cornea.
Keratoconus Screening involves various eye tests to detect the condition early, allowing for timely intervention and treatment to prevent or slow its progression. Some common screening tests to diagnose keratoconus include:
- Eye refraction: Check eye’s refractive power which offers the sharpest vision and detect vision problems with special tools, devices and equipment.
- Slit-lamp examination: Directing a vertical beam of light on the surface of the eye and using a low-powered microscope to evaluate the cornea shape and detect any other potential eye problems.
- Keratometry: A diagnostic test to measure the curvature of the cornea. It is usually done in combination with eye refraction in order to determine the power of a corrective lens that will be needed to correct vision.
- Computerized corneal mapping: Special photographic tests like corneal topography and optical coherence tomography which record cornea thickness and images to create a detailed map of your cornea shape and surface.
Who Needs Screening?
- Those with a family history of keratoconus.
- Children of parents with keratoconus should get their eyes checked for signs every year, starting at age 10.
- Those experiencing vision changes, such as blurred vision, frequent changes in eyeglass prescriptions, or increased sensitivity to light.
- Those with progressive myopia or significant astigmatism.
Treatment
In the early stages of keratoconus, eyeglasses and soft contact lenses may help to correct blurry or distorted vision. In some cases, specialized contact lenses may help to correct corneal curvature and improve vision. In more progressive cases, surgical options, such as, corneal inserts corneal cross-linking and cornea transplants, may be necessary to halt corneal scarring and thinning.
Cataract Screening
Cataract is a congenital or degenerative opacity of the lens inside your eyes which can happen in one or both eyes. It usually develops slowly over several years with gradual vision blurring, loss of contrast and reduced visibility in low light condition which may not be noticeable at first. Cataract is very common and rarely serious, but it can affect your daily life in many ways.
Cataract Screening is a diagnostic procedure performed by an eye doctor and/or clinical optometrist to detect the presence of cataracts. The screening typically involves a comprehensive eye examination, including visual acuity test, slit-lamp exam, and retinal exam (back of the eye). It is an important part of maintaining visual health especially after the age of 40. It should be done every two years after age 40 and every year after age 65.
If detected early enough, the following interim measures are recommended without the need cataract surgery right away:
- Regular eye exam to update prescription and if necessary, change the lenses and contact lenses with the new prescription.
- Choose lenses with anti-glare coating.
- Use brighter lightings at home and workplace.
- Use a magnifying glass to read printed text.
- Increase the font size on the phone or computer.
Cataract Prevention
Some preventive measures may help reduce the risk of cataracts and may protect the overall eye health:
- Wear sunglasses with UV 400 and/or a hat with a brim to block the sun.
- Wear protective eyewear or safety glasses if you are in a high-risk activity.
- Healthy diet rich in antioxidants may reduce the risk of cataracts. Nutrients like vitamins A, C, E, astaxanthin, lutein and zeaxanthin are linked to eye health.
- Avoid excessive alcohol consumption which increases the risk of cataracts.
- Manage blood sugar levels – high blood sugar levels can cause Diabetic Retinopathy, a complication of diabetes, which damages the retina (back of the eye) and results in blindness if left untreated.
- Quite smoking – Smoking increases the production of free radicals in the body, which can damage the eye’s lens and contribute to cataract formation.
